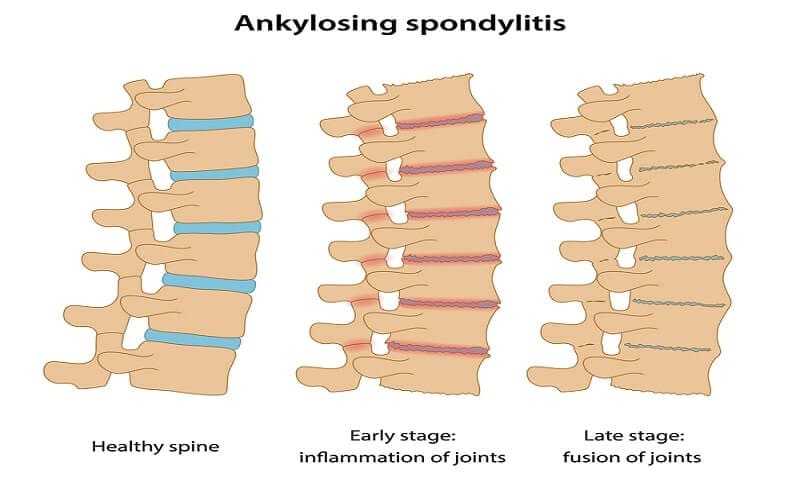
Does Having the Antigen HLA-B27 Assumes With Ankylosing Spondylitis?

A small minority of people with this disease suffer antigen, even taking family with ankylosing spondylitis.
Most people in whom it develops ankylosing spondylitis are previously healthy, however, other diseases with similar behavior called spondyloarthropathies, may occur in people with inflammatory bowel disorders, urinary tract infections or illness of the skin called psoriasis.
What are the symptoms of ankylosing spondylitis? Ankylosing spondylitis is a rare disease. It appears in young people, especially in males between 20 and 30.
However, some cases may begin in childhood or adolescence, and affect women, although in these the disease is usually milder and is often more difficult to diagnose.
Signs that may indicate the condition of ankylosing spondylitis:
1. Pain onset before age 35.
2. Spine stiffness in the morning, on rising from bed.
3. Improvement of symptoms with activity.
4. Sub acute onset or poorly defined.
5. Duration of symptoms greater than 3 months.
The first thing to note the person with ankylosing spondylitis is usually lumbar or low back pain, which is produced by inflammation of the joints sacroiliac and vertebral. This pain is inflammatory, and manifests itself insidiously, slowly, slowly, unable to pinpoint the moment that the symptom started. Low back pain occurs when the patient is at rest, improving physical activity. This pain is often hard in the final hours of the night and early in the morning, when the patient takes a long time in bed. In these circumstances, this symptom requires the person to get up and walk to notice a relief and even disappearance pain.
Given this inflammatory pain of ankylosing spondylitis is another lumbago mechanical origin of sudden onset that is either located by the patient in a particular area of the spine, improves with rest and worsens with.
The human leukocyte antigen (HLA B27) is found in 5-10% of the U.S. population and is often associated with various autoimmune diseases. The most common is ankylosing spondylitis (AS).
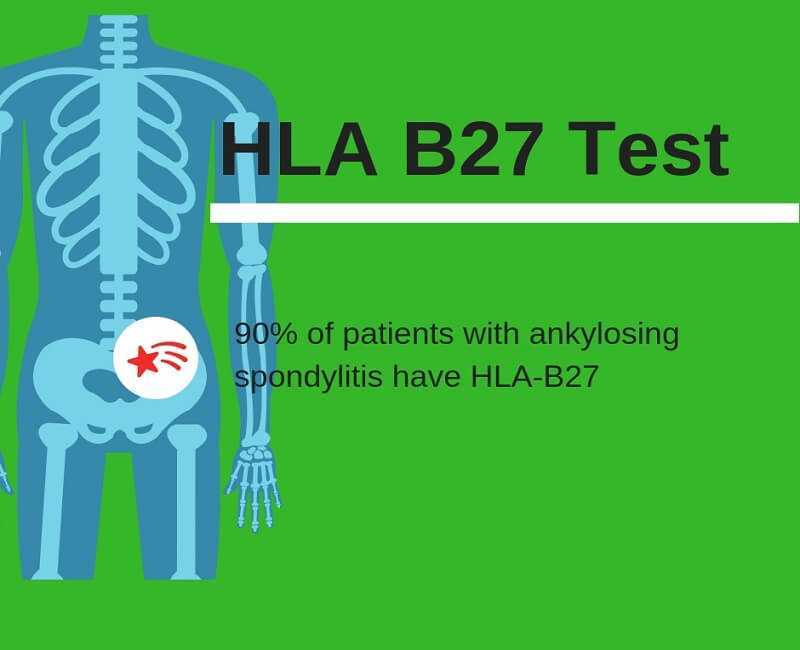
About 90% of patients with AS are HLA B27 positive. Other autoimmune diseases are associated juvenile rheumatoid arthritis (80% of patients), and Reiter’s syndrome or reactive arthritis (50-80%).
The HLA B27 is also present in 50% of patients with inflammatory bowel disease and psoriasis with ankylosing spondylitis. The HLA B27 is not the cause of these pathologies, but there is a higher prevalence of this antigen in affected patients.
Is there anything else I should know? If one of his members of the family has a spondyloarthropathy with HLA B27 positive (AS or other) and you also have the HLA B27 positive has more risk of developing a spondyloarthropathy.
What is the result? HLA B27 can be positive or negative. If positive, HLA B27 (structural protein) is present in the membrane of nucleated cells of the body, including leukocytes. If, in addition to HLA B27, there are symptoms such as chronic pain and inflammation or degenerative bone changes (visible in radiography), it is likely that the patient has AD, Reiter’s syndrome or other autoimmune disease associated with HLA B27. This is more likely if the patient is a young man who began having symptoms before age 40.
HLA B27 can also be seen in other autoimmune diseases such as:
* Isolated acute anterior uveitis
* spondiloartropatias idiopathic
* Synovitis enteropathica
If B27 is negative, the less likely the symptoms are due to an autoimmune condition associated with this antigen. (There are exceptions, since 10% of the AS and 40-50% of Reiter’s syndrome is HLA B27 negative).
Currently, the act of detecting the antigen is not indicative of developing an autoimmune disease, because if the patient does not have any symptoms associated with the presence of antigen does not allow us to say that illness is, how quickly they evolve, their severity, prognosis or extent of organ involvement.
Facebook
Google+
Twitter
Pinterest
Reddit
StumbleUpon